Age-Related Macular Degeneration
Macular degeneration is a deterioration or breakdown of the macula. The macula is a small area in the retina at the back of the eye that allows you to see fine details clearly and perform activities such as reading and driving. When the macula does not function correctly, your central vision can be affected by blurriness, dark areas or distortion. Macular degeneration affects your ability to see near and far, and can make some activities—-like threading a needle or reading—difficult or impossible.
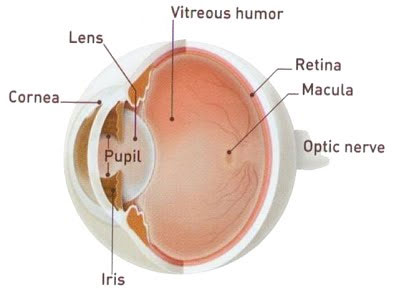
Although macular degeneration reduces vision in the central part of the retina, it usually does not affect the eye’s peripheral or side vision. For example, you could see the outline of a clock but not be able to tell what time it is.
Macular degeneration alone does not result in total blindness. Even in more advanced cases, people continue to have some useful vision and are often able to take care of themselves. In many cases, macular degeneration’s impact on your vision can be minimal.
What Causes Macular Degeneration?
Many older people develop macular degeneration as a part of the body’s natural aging process. There are different kinds of macular problems, but the most common is age-related macular degeneration (AMD). Exactly why it develops is not known, and no treatment has been uniformly effective. Macular degeneration is the leading cause of severe vision loss in Caucasians over 65.
The two most common types of AMD are “dry” (atrophic) and “wet” (exudative).
“Dry” Macular Degeneration (Atrophic)
Most people have the “dry” form of AMD. It is caused by aging and thinning of the tissues of the macula. Vision loss is usually gradual.
“Wet” Macular Degeneration (Exudative)
The “wet” form of macular degeneration accounts for about 10% of all AMD cases. It results when abnormal blood vessels form underneath the retina at the back of the eye. These new blood vessels leak fluid or blood and blur central vision. Vision loss may be rapid and severe.
Deposits under the retina called drusen are a common feature of macular degeneration. Drusen alone usually do not cause vision loss, but when they increase in size or number, this generally indicates an increased risk of developing advanced AMD. People at risk for developing advanced AMD have significant drusen, prominent dry AMD, or abnormal blood vessels under the macular in one eye (“wet” form).
What are the symptoms of macular degeneration?
Macular degeneration can cause different symptoms in different people. The condition may be hardly noticeable in its early stages. Sometimes only one eye loses vision while the other eye continues to see well for many years. But when both eyes are affected, the loss of central vision may be noticed more quickly.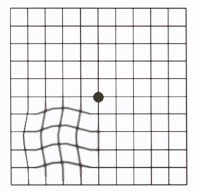
Following are some common ways vision loss is detected:
- words on a page look blurred
- a dark or empty area appears in the center of vision
- straight lines look distorted
How is macular degeneration diagnosed?
Many people do not realize that they have a macular problem until blurred vision becomes obvious. Your ophthalmologist (Eye M.D.) can detect early signs of AMD during a medical eye examination that includes the following:
- a simple vision test in which you look at a chart that resembles graph paper (Amsler grid)
- viewing the macula with an ophthalmoscope
- taking special photographs of the eye called fluorescein angiography to find abnormal blood vessels under the retina
How is macular degeneration treated?
Nutritional Supplements
Although the exact causes of macular degeneration are not fully understood, antioxidant vitamins and zinc may reduce the impact of AMD in some people.
A large scientific study found that people at risk for developing AMD lowered their risk by about 25% when treated with a high-dose combination of vitamin C, vitamin E, beta carotene and zinc. Among those who have either no AMD or very early AMD the supplement did not appear to provide an apparent benefit.
It is very important to remember that vitamin supplements are not a cure for AMD, nor will they restore vision that you may have already lost from the disease. However, specific amounts of these supplements do play a key role in helping some people at risk for advanced AMD to maintain their vision. You should speak with your ophthalmologist to determine if you are at risk for developing advanced AMD, and to learn if supplements are recommended for you.
Laser Surgery, PDT and Anti-VEGF Treatments
Certain types of “wet” macular degeneration can be treated with laser surgery, a brief outpatient procedure that uses a focused beam of light to slow or stop leaking blood vessels that damage the macula. A treatment called photodynamic therapy (PDT) uses a combination of a special drug and laser treatment to slow or stop leaking blood vessels.
Another form of treatment targets a specific chemical in your body that is critical in causing abnormal blood vessels to grow under the retina. The chemical is called vascular endothelial growth factor (VEGF). Anti-VEFT drugs block the trouble-causing VEGF, reducing the growth of abnormal blood vessels and slowing their leakage.
These procedures may preserve more sight overall, though they are not cures that restore vision to normal. Despite advanced medical treatment, many people with macular degeneration still experience some vision loss. Early detection and treatment may minimize vision loss.
Injections
Wet AMD can now be treated with new drugs that are injected into the eye (anti-VEGF therapy). Abnormally high levels of a specific growth factor occur in eyes with wet AMD and promote the growth of abnormal new blood vessels. This drug treatment blocks the effects of the growth factor.
You will need multiple injections that may be given as often as monthly. The eye is numbed before each injection. After the injection, you will remain in the doctor’s office for a while and your eye will be monitored. This drug treatment can help slow down vision loss from AMD and in some cases improve sight.
Adapting to Low Vision
To help you adapt to lower vision levels, your ophthalmologist can prescribe optical devices or refer you to a low-vision specialist or center. A wide range of support services and rehabilitation programs are also available to help people with macular degeneration maintain a satisfying lifestyle. Because side vision is usually not affected, a person’s remaining sight is very useful. Often, people can continue with many of their favorite activities by using low-vision optical devices.
Resources
For more information, please contact
The American Academy of Ophthalmology
415.561.8500
www.aao.org
The American Macular Degeneration Foundation
413.268.7660
www.macular.org
Foundation Fighting Blindness
800.683.5555
800.683.5551 TDD
www.FightBlindness.org
Macular Degeneration. A Closer Look. (2007). American Academy of Ophthalmology. San Francisco, CA.
Amsler Grid Testing
Click here to print your own Amsler Grid
- A BRIEF REMINDER: Hold the card 14 inches from your eyes. Wear your glasses if needed for reading.
- Cover one eye, look at the center dot with the uncovered eye, keep your vision fixated on that dot, note any visual distortion using your side/peripheral vision, then repeat this procedure using your other eye.
- If the lines look irregular (wavy, blurred, empty, or discolored), promptly call our office.
Take an Eye Vitamin: AREDS
Check the bottle for how many to take daily.
Click here to print an informational handout on eye vitamins.
Diet and Risk of Age-Related Macular Degeneration
High dietary intake of Betacarotene, Zinc, and Vitamins C and E reduce risk of AMD by 35%.
Whole grains, vegetable oil, eggs, and nuts
(Sources of Vitamin E)
Meat, poultry, fish, whole grains, and dairy products
(Sources of Zinc)
Carrots, kale, and spinach
(Sources of beta-carotene)
Citrus fruits and juices, green peppers, broccoli, and potatoes
(Sources of Vitamin C)



